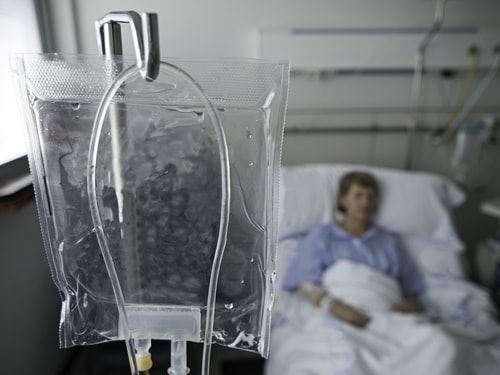
The coronavirus pandemic spiked first in March, raising immediate concerns about what it could do to the nation’s elderly population. By late November, more than 90,000 elders living in nursing homes and assisted living centers had died due to COVID-19 complications and symptoms. As harrowing as this statistic might be, the Associated Press (AP) warns that tens of thousands more elders in nursing homes have likely died of neglect and abuse caused by staff members during the pandemic. The heightened stress and demands of attempting to control the coronavirus’s spread in nursing homes have been mostly blamed for the spike in abuse-related nursing home deaths.
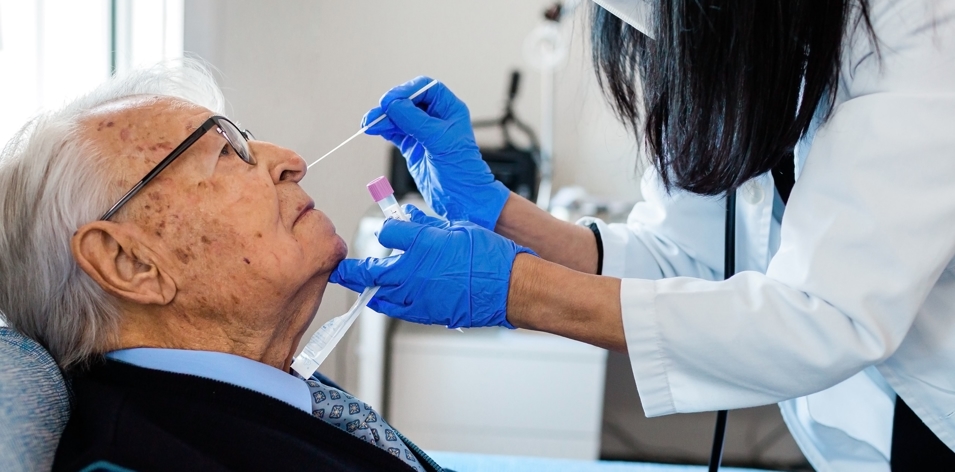
According to the Associated Press researchers, an elderly care expert who used data from 15,000 nursing home centers determined that while 90,000 elders have died from COVID-19 in nursing homes, another 45,000 or so have died from preventable neglect in nursing homes during the same span of time.
Furthermore, the additional deaths are not even counting the expected mortality rate in nursing homes, such as from old age and other illnesses. Overall, the non-COVID-related elderly deaths in nursing homes have increased by at least 15% by the researchers’ approximations.
Doubling Death Rates Once the Virus Spreads
Stephen Kaye is a professor at the Institute on Health and Aging at UC San Francisco. He was interviewed by Associated Press and assisted with their research. Based on his findings, non-COVID-related nursing home deaths would double as soon as the coronavirus was positively identified in 3 or more residents.
Issues that could be causing other abuse or neglect related deaths once the virus enters a nursing home are:
- Understaffing: A nursing home resident who has contracted the coronavirus could need at least twice as much attention as another resident without it by some estimates. Even if all nursing home staff members and caretakers are able to stay working full-time during a virus outbreak, they will be faced with significantly more daily demands than normal. However, once a staff member contracts the virus, they and many others in the workforce need to isolate for two weeks or longer, which only compounds the understaffing issue. In any circumstance, the AP researchers found that an inordinate amount of nursing home residents were not getting the day-to-day care they needed.
- Exhaustion: An exhausted caretaker cannot provide the same quality of care that a well-rested one can. There are no two ways around that issue. As the pandemic continues and worsens, hardworking caretakers who genuinely want the best for the residents under their care will eventually become too fatigued to continue working as normal.
- Overprotective care: There is also the issue of caretakers becoming overprotective of vulnerable residents to the point that they do more harm than good. For example, a caretaker might believe that they need to spend less time with a resident who has not been diagnosed with COVID-19 out of fear that staying within proximity of them for long will increase the chances of giving them the virus if they, the caretaker, are asymptomatic or pre-symptomatic. While this might be true, it is not a reason to stop giving an elderly nursing home resident regular amounts of care and attention, especially if the change in care causes problems like dehydration and emotional isolation.
American Health Care Association Argues Otherwise
A representative from the American Health Care Association (AHCA) has said that there is insufficient evidence to suggest that the coronavirus has caused a dip in day-to-day care for elderly nursing home residents, though. According to this group, new admissions to nursing homes and assisted living centers have plummeted in many regions due to fear of the virus spreading throughout those facilities. Therefore, based on that claim, the care demand increase caused by the virus could be counterbalanced by there being fewer residents who need care overall.
Another argument has been made that the unavoidable drop or elimination of familial visitations in nursing homes has worsened the situation in a way outside of nursing home staff control. Most family members who visit a loved one in a nursing home actually help with their care, even in small ways, such as helping with meals or just spending time with them to boost their spirits. With nursing homes locking down in March 2020 and banning essentially all visits, countless little “tasks” once handled by visiting families were suddenly dumped onto the shoulders of caretakers.
Who is to Blame & What Can Be Done?
Lawsuits against nursing homes for COVID-19 fatalities and other neglect-related deaths during the pandemic are going to be rocky, to say the least. Many nursing homes have already sought legal immunity from liability if a resident dies due to the coronavirus because the virus is currently so prevalent across the country. Others have posed similar arguments as the AHCA, saying that the connection between the increase in neglect-related resident deaths and the spread of the coronavirus is tentative at best and that those deaths would have occurred anyway in any situation.
What is known is that when more families of elderly nursing home residents do decide to take legal action for the wrongful deaths, there could be a massive influx of claims and lawsuits filed in a short amount of time. It might even become necessary for some of the claims to be consolidated into a class action or mass tort. For each of the 130,000 – and counting – COVID-related nursing home deaths, there are that many families at least who are left mourning and seeking answers and justice.
The Gatti Law Firm is a leading nursing home abuse law firm for plaintiffs in Oregon. Visit our blog often for important updates about nursing home death news stories and lawsuits, especially for those pertaining to the ongoing coronavirus pandemic. If you think you need our firm’s help for a claim of your own, then please fill out an online contact form at your first opportunity.
 Get Free Case Evaluation
Get Free Case Evaluation